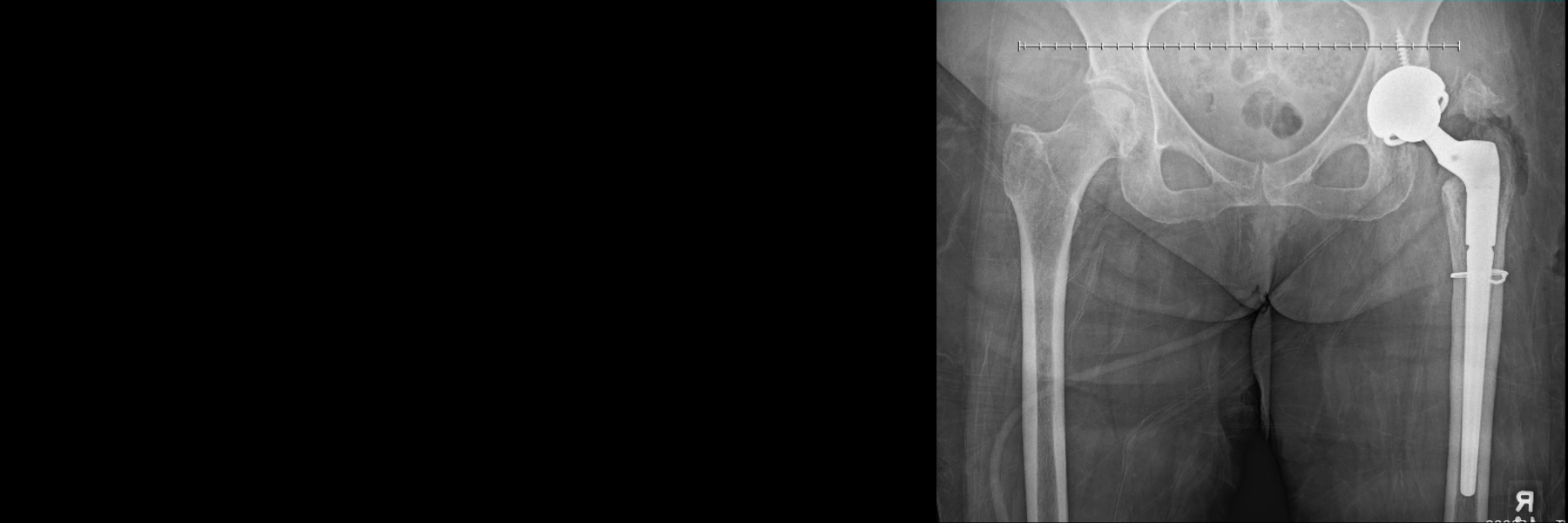
Revision Hip and Knee Replacement
Indications for Revision Hip or Knee Replacement
Although hip and knee replacement continue to be two of the most successful interventions in modern medicine, there are occasional cases in which patients are unsatisfied with their outcome. The reasons therein may be related to implant, surgical, or patient-related factors.
If the patient has a joint replacement that is not functioning adequately, usually the underlying cause can be detected through a thorough history and physical exam, appropriate imaging and laboratory workup, and knowledge of the implant type and known performance over time.
In many cases, further surgery may not be required, but rather the patient can be treated with physical therapy, activity modification, or medications. However, if there is a more serious problem with the joint, it may rarely require revision surgery to fix the problem.
Historical Perspective and Prevention of Complications
Critically important to ensuring good outcomes after joint replacement surgery is adequate surgical planning, proper patient selection, appropriate patient education, and pre-operative patient optimization. Many potential complications can be anticipated and addressed prior to surgery, in order to ensure that the patient has a smooth recovery.
For example, high-risk patients such as those with morbid obesity, diabetes, neurogenic problems, or kidney disease can often be optimized pre-operatively with the help of a medical doctor, making them better candidates for surgery and lowering the likelihood of any need for future revision.
Choice of Surgical Approach, Technique, and Implant
Depending on the particular issue with the joint, the surgeon may opt to revise the implant through the same surgical approach, utilizing the previous incision, or they may elect to make a new incision in a different location and use a separate approach.
Much of this decision making has to do with the exposure necessary to perform the revision, the instrumentation needed to get the old implant out and put the new implant in, and the degree of bone loss or soft tissue damage that is anticipated. Ultimately the surgical approach, revision technique, and implant type are chosen on a case-by-case basis depending on the specific needs of the patient.
Post-Operative Recovery
After revision of a total joint replacement, the recovery protocol may vary substantially depending on what type of revision was performed, the type of implant that was placed, and the degree of bone loss or soft tissue damage that was discovered intra-operatively.
In some cases, patients may have relatively few restrictions on their activity, and physical therapy may proceed similarly to a primary total joint replacement.
However, a more extensive revision may require that significant restrictions on weight bearing or motion to be placed on the patient for the first several weeks of the recovery.