Total Hip Replacement
Indications for Total Hip Replacement
There are a variety of conditions which may result in a worn-out hip joint. Most common is osteoarthritis, a “wear-and-tear” condition in which the protective cartilage covering of the joint gradually thins out over time, resulting in progressive hip pain and stiffness.
More rarely seen are the inflammatory types of arthritis, such as rheumatoid arthritis, which is a medical condition resulting in progressive cartilage loss. Previous injury or deformity to the hip results in changes to the local biomechanical properties of the joint, which may accelerate cartilage loss.
Another common reason for hip replacement is avascular necrosis, a condition in which the hip loses its blood supply, gradually resulting in the collapse of the joint with concurrent loss of cartilage.
When the joint damage has become sufficiently severe, and the patient’s quality of life is beginning to suffer, a total hip replacement may be indicated.
Historical Perspective
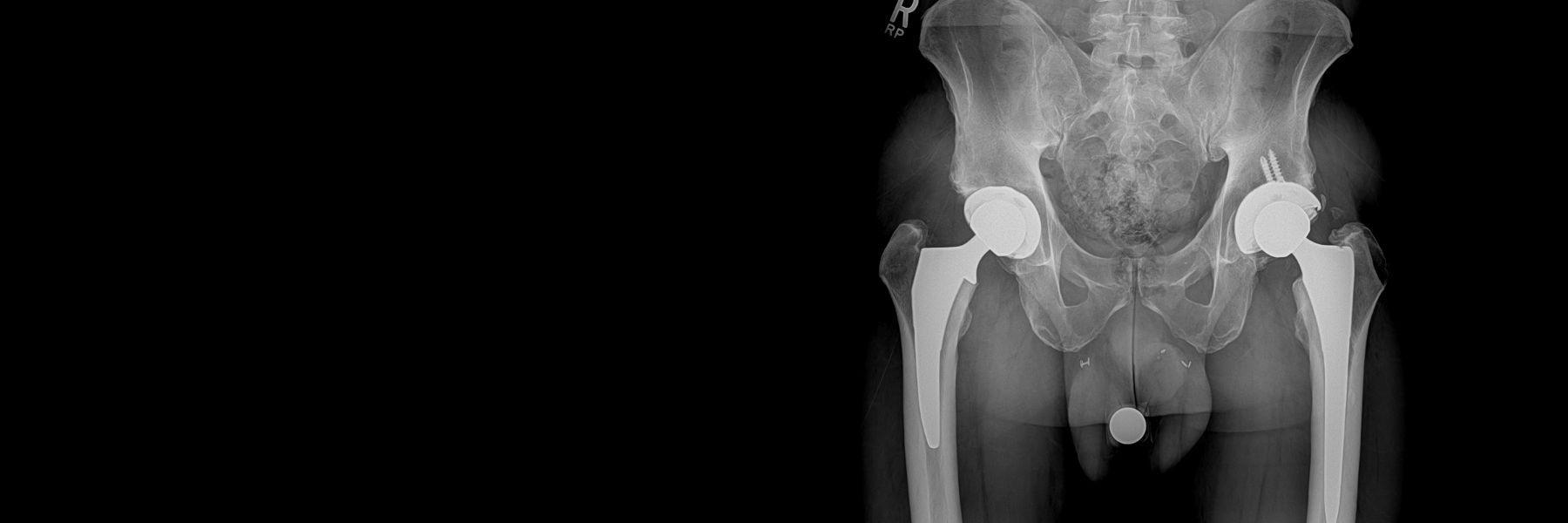
Total hip replacement surgery is a tremendously successful procedure for eliminating pain and restoring function in patients with severe hip arthritis. Most simply put, a total hip replacement involves removal of the damaged cartilage and bone from the ball and socket of the patient’s arthritic hip and replacing these with a new ball-and-socket implant that allows the patient to walk with smooth motion and without pain.
Historically, a variety of dissection techniques (called surgical approaches) have been used to gain access to the hip joint. Each of these approaches has its own advantages and drawbacks. Most recently, the Direct Anterior Approach, which has been highly utilized in Europe for many years, has gained increasing popularity over the last decade in the United States.
A Minimally Invasive Technique
The Direct Anterior Approach utilizes an intermuscular plane of dissection, meaning no muscles or tendons need to be cut during the surgery. Because of this preservation of the soft tissues, patients do not require any hip precautions or restrictions during their rehabilitation period. Immediate weight bearing as tolerated is prescribed, with no restrictions.
Surgical Technique: Patient Positioning, Limb Control, and Fluoroscopy-Assisted Computer Navigation
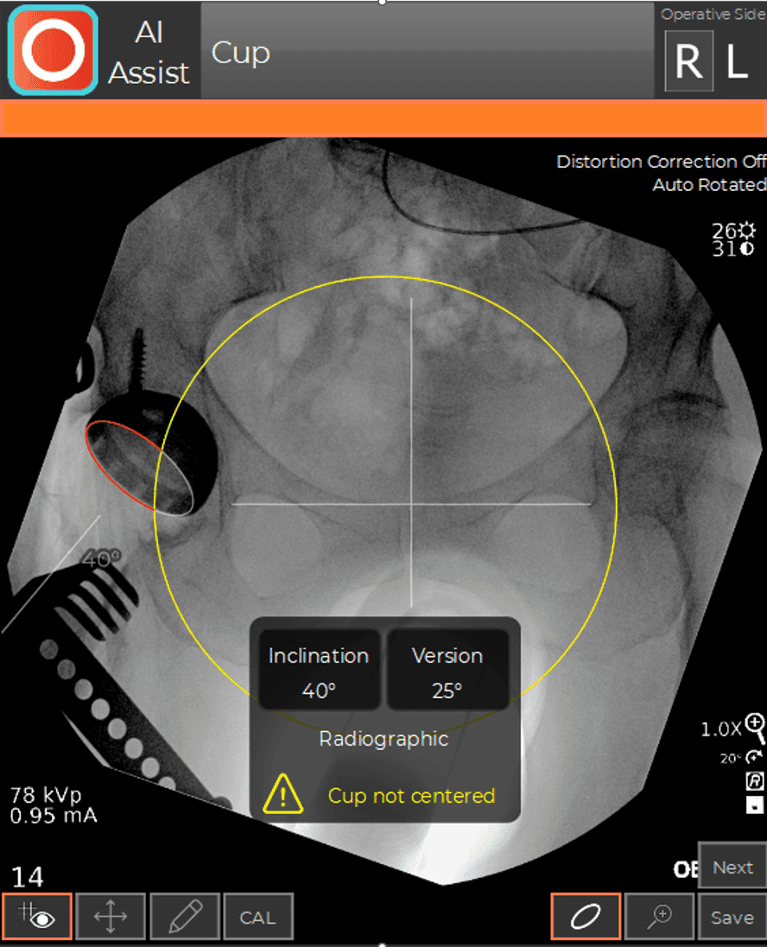
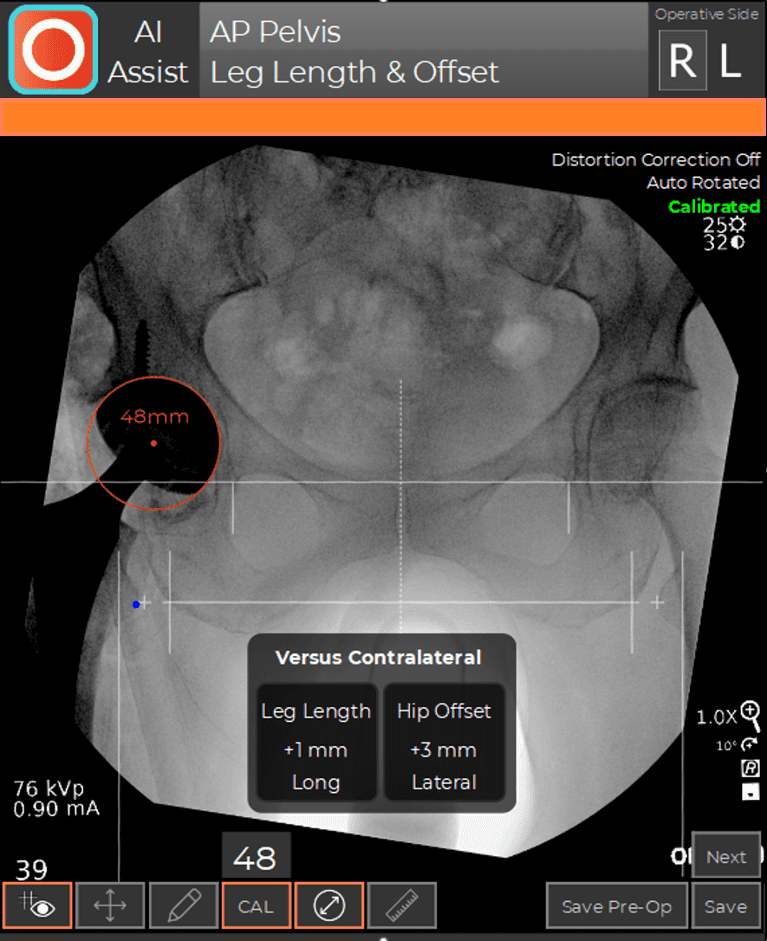
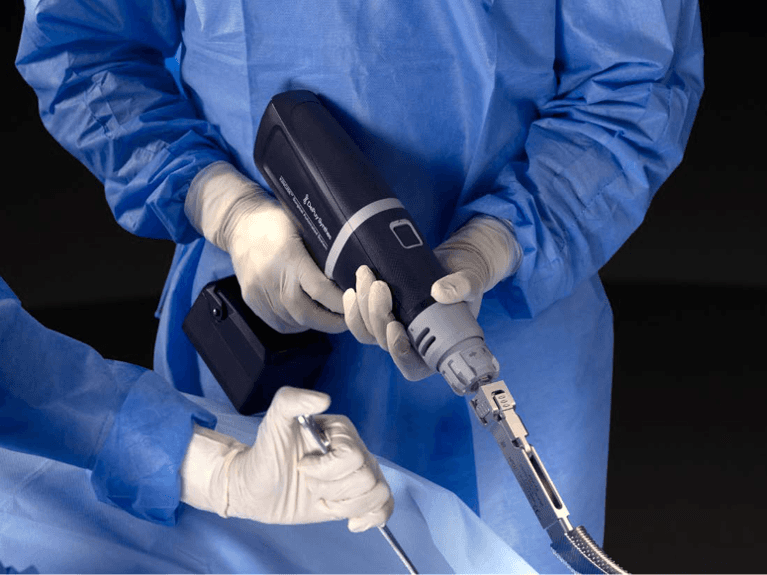
During a hip replacement using the Direct Anterior Approach, the patient is positioned supine on a traction table (the Hana® table) that allows independent positioning of the limbs during surgery. This position facilitates the use of C-arm fluoroscopy. C-arm fluoroscopy is an intra-operative x-ray camera that projects images on a computer monitor in the operating room and is used to navigate the position of the hip socket and stem in real-time during the procedure. The fluoroscopic images are analyzed by computer software (OrthoGrid Systems, Inc.), which registers multiple anatomic landmarks in order to calculate socket position, leg length, and offset. This allows the surgeon to make small adjustments intra-operatively, in order to ensure an anatomic reconstruction.

Post-Operative Recovery
After a direct anterior total hip replacement, patients may immediately weight bear as tolerated, with no restrictions. Specific physical therapy protocols are available on the website and will be initiated by your physical therapist.
For the first 2-4 weeks, patients are encouraged to walk, practice going up and down stairs, and generally resume the activities of daily living.
By 2-4 weeks, most patients have discontinued the need for a cane and are walking unsupported.
From 6-12 weeks, the patient will notice larger gains in physical therapy in terms of endurance, range of motion, and strength.
Usually by 12 weeks, the patient is starting to feel close to normal and is resuming most activities, but many patients continue to see ongoing improvement even up through one year after surgery.